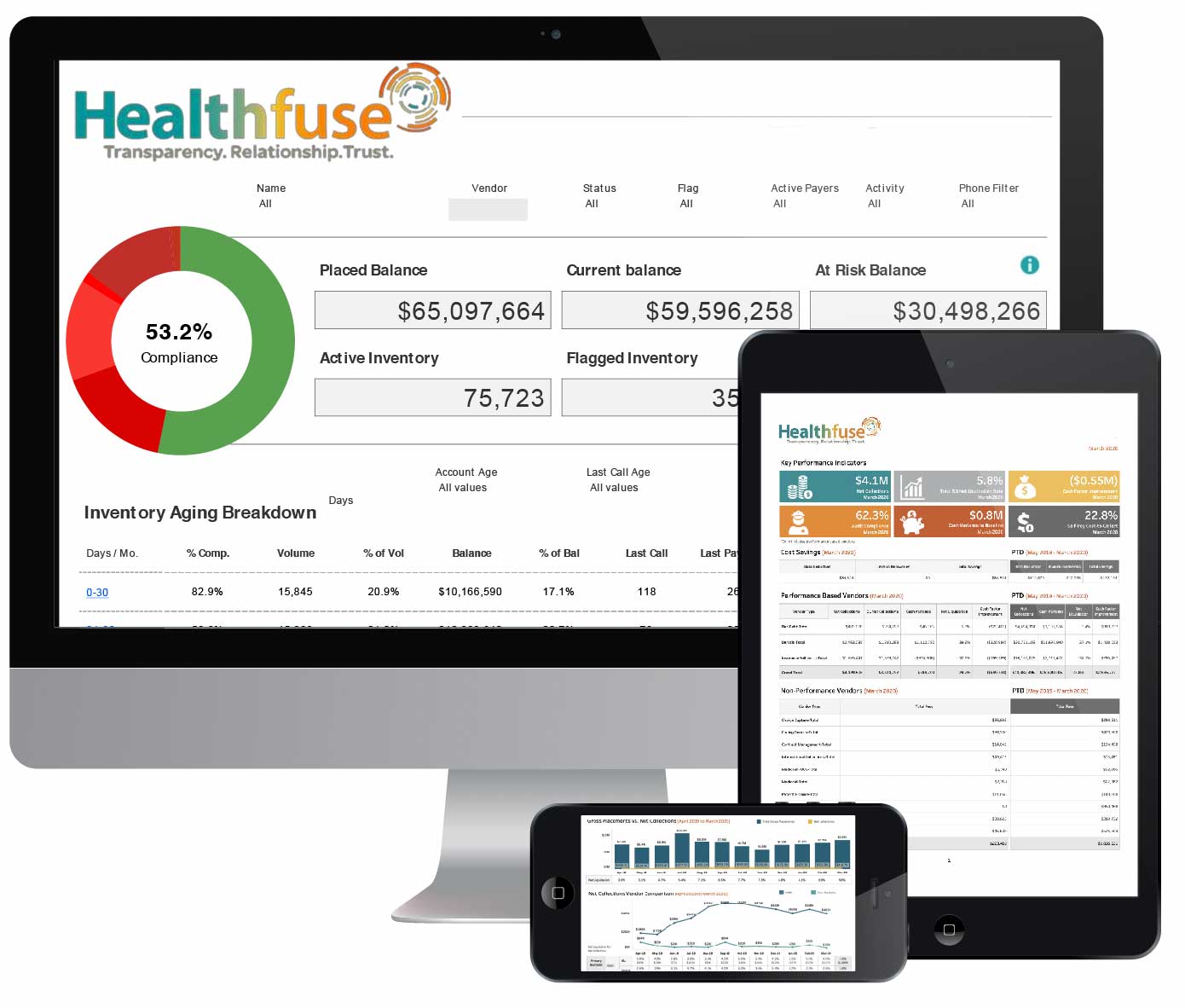
Revenue Cycle
Vendor Management
WITH GUARANTEED BOTTOM-LINE RESULTS
Get the most from your vendor partnerships with the only tech-enabled vendor management program that guarantees cost savings and collections improvement for your hospital.
$1 Billion
300+
100%


Develop and Source
Benchmark and Analyze
Vendor data and insights from 3,000+ vendors and hospitals


Negotiate and Implement
Discover and Recover
Invoice dupes and fees and
strengthen contracts and SLAs


Measure and Report
Automate and Reconcile
Inventory, track vendor ROI in real-time dashboards/scorecards
Why Healthfuse
Revenue Cycle Vendor Accountability
The pandemic created a financial crisis for hospitals. Revenue cycle teams had to adapt quickly, redeploying staff and relying on vendors to fill the gaps.
Hold Your Vendors Accountable
Our end-to-end, tech-enabled approach, combined with a dedicated execution team, provides revenue cycle teams with:
- 100% vendor transparency
- Accelerated cost savings
- Improved collections
- Guaranteed bottom-line results